The Cass Paradox
By Stella O'Malley

In this essay I argue that medical transition lacks a reliable evidence base and that focusing solely on paediatric cases concedes the central argument
I call it the Cass Paradox. After four years reviewing the evidence for the medicalisation of children’s identities, Dr Hilary Cass and her team found no reliable evidence of benefit for interventions that carry risks of infertility, sexual impairment, and significant physical harm. These are consequences children are inherently too immature to fully understand. Yet Dr Cass remains open to the idea that some children may benefit, and this openness has contributed to confusion about the wider issue. The Cass Paradox highlights a review that finds no reliable evidence of benefit yet still refuses to rule out the intervention.
This inability to close the door is striking. Across clinicians and researchers who describe themselves as “gender critical” but are better named “gender critical lite”, there remains a refusal to fully say no to medical transition. They tend to subscribe to an unevidenced theory – I have a name for this too – the “tiny numbers theory”; the belief that a vanishingly small group might benefit, despite the absence of evidence.
As a basis for healthcare, this is farcical. Treatments are not justified by the possibility that someone, somewhere, might benefit. The burden of proof rests with those making the claim, yet here it is inverted and sustained through self-report and speculation. The gender critical lite crowd cannot seem to move on from this thinking, insisting on focusing narrowly on the risks of paediatric medical transition while avoiding the larger and more important question of medical transition itself.
Most people, even those with little knowledge of this issue, recognise that paediatric medical transition is a reckless and inappropriate intervention. Dr Cass is internally inconsistent in this respect, and one cannot help but think she has been politically outmanoeuvred, as seen with the shenanigans over the puberty blocker trial. It came as no surprise when the data linkage study shifted from being deemed impossible to carry out to suddenly being approved; there has clearly been significant institutional pressure in this space.
In the meantime, self-report is relied upon to keep the door ajar for medical transition for a “tiny number” of people. Even though this is not a basis for standard healthcare; self-report is inherently unreliable and does not justify medical intervention.
As Bertrand Russell illustrated, we cannot prove that a teapot, too small to be seen by telescopes, orbits the Sun somewhere between the Earth and Mars. But the fact that we cannot disprove the claim does not make it credible, nor does it justify action. Thankfully, the standards for ethical treatment are higher than that. It is not enough that a small section of people tell us that homeopathy is wonderful – it will not be accepted as appropriate treatment until it is supported by robust, replicable evidence demonstrating clear and reliable benefit.
By focusing solely on paediatric cases, researchers inadvertently legitimise adult medical transition. It is beyond time for this issue to be confronted with clarity and leadership. Obfuscation and an apologetic demeanour are creating confusion and chaos in wider society. Most people who are not in the field presume that there is a substantial and reliable evidence base for adult medical transition, just not for paediatric transition.
When exactly should we tell them there isn’t?
Presenting medical transition as a feasible healthcare treatment for adults causes harm – just ask Ritchie Herron or Sinéad Watson or any of the 600 detransitioners who have taken part in our Beyond Trans programme. The truth is, as anyone who has studied this issue knows, if we are to be objective, the long-term outcomes of trans-medicalisation have repeatedly failed to demonstrate benefit.

In 1979 Mayer and Reter compared a group of individuals who sought sex reassignment surgery but did not receive it with a group who medically transitioned. They concluded that “sex reassignment surgery confers no objective advantage in terms of social rehabilitation”. Consequently, the Gender Identity Clinic at Johns Hopkins made the decision to no longer offer sex reassignment surgery, then the treatment of choice for this cohort.
Little has changed in the peer-reviewed outcomes since then. But today, in this era of hyper-medicalisation, over-diagnosis, and patient-led care, the rise of an individualistic, post-modern self means that a subjective sense of identity is now treated as sufficient grounds for medical intervention.
The difference between now and then is that Meyer and Reter relied on objective outcome measures rather than subjective, self-reported accounts of an unfalsifiable sense of inner wellbeing. They examined externally observable outcomes – employment status, relationships, social functioning, psychiatric treatment, hospitalisation, and general social adjustment.
Kuiper and Cohen-Kettenis (1991) also reported poor outcomes in their study of 141 Dutch transsexuals, including a 70% loss to follow-up and 12 deaths among 105 male participants. Then in 2011, Dhejne et al. conducted the longest follow-up study to date on the outcomes of “sex reassignment surgery”, covering 30 years (1973-2003) and involving 324 individuals in Sweden. Compared with matched controls based on birth year and sex, those who had undergone surgery had a significantly increased risk of death by suicide, with rates over 19 times higher than controls. They also showed elevated rates of suicide attempts and psychiatric inpatient care. The data further indicated higher rates of criminal involvement and significant substance misuse.

Paediatric medical transition has undergone even less scrutiny than adult transition – largely because, until recently, it was considered a pretty insane idea. Only in the past twenty years has it been attempted and it is only now that the evidence is emerging. The Cass Review concluded that the evidence base for medical transition in children and adolescents is very weak and uncertain. There is insufficient high-quality evidence to support this experimental treatment, and clinical practice has moved ahead of the evidence despite known and potential risks.
Just yesterday, it came as no surprise to anyone in this field that a new Finnish study reported that medical transition for those under 23 did not improve mental health. Psychiatric morbidity rose sharply, from around 10% to over 60% in male-to-female adolescents, and from around 22% to over 54% in female-to-male patients. As the study states, “Severe psychiatric morbidity is common among gender-referred adolescents… Psychiatric needs do not subside after medical gender reassignment.”
We know that this treatment approach is profoundly inappropriate for these vulnerable patients. Yet many still cannot state clearly and unapologetically that these interventions are wrong. The harms extend beyond the individual to families, workplaces, and wider society. Nonetheless, Dr Cass and many others continue to insist the door must remain slightly ajar.
It is this very reluctance to close the door that has created the current situation. Even in Ireland, where the National Gender Services always rejected WPATH and the gender-affirmative model, services have been overwhelmed by the new rapid-onset gender dysphoria (ROGD) cohort.
Until the ROGD cohort began presenting in clinics in the early 2010s, the NGS operated a small service for the vanishingly few who sought medical transition, with a strong emphasis on safeguarding and preventing unnecessary interventions. Even so, it remained an inappropriate treatment pathway.
It is important to note that clinicians in the NGS, like Cass, do not subscribe to the concept of “true trans”. Instead, “tiny numbers theory” rests on the belief that a very small group may benefit from medicalisation, and that these individuals are identifiable by highly skilled clinicians. Their focus is not on identity claims but on outcomes. The problem is that objective measures are being steadily replaced by subjective, post-modern reliance on self-report, and the skills of these clinicians have been called into question by the growing number of people who regret their medical transition.
This approach has been studied since the 1960s, yet we still lack robust evidence to support it. Nobody has managed to prove that the teapot is circling the Sun. At what point do we accept that these interventions are too radical and too damaging to uphold?

Isn’t it time that those of us who are fully informed state this clearly and without apology – that this is not an appropriate intervention, that it causes more harm than any discernible self-reported benefit, and that its effects extend beyond the individual into family distress and wider social disruption?
Families of trans-identified people are seldom studied. However, with over 5000 family members having engaged with our Beyond Trans network, a clear pattern has emerged. The impact on families is comparable to living with anorexia or OCD; it is extremely difficult for everyone.
I often wonder what would have happened if children had not presented with ROGD. The trans industry could have expanded unchecked, and the evidence base might never have been tested. It was parents who exposed this pseudo-medical intervention for what it is – more flawed than homeopathy and even more extreme in concept.
It turns out that when medical interventions are performed on children, parents will go to the ends of the earth to understand what is being proposed. In this case, they did. These parents have gone through hell, only to discover that the clinicians and researchers were asleep at the wheel. The research base has been weakened by self-report, poor-quality studies, and a lack of replication. This field is littered with weak evidence. When the parents arrived in their droves, they examined the data and they are now saying “No” – loudly, clearly, and unapologetically.
The genie is out of the bottle. Just as anorexia, bulimia, and self-harm were once extremely rare, gender dysphoria is now becoming another pathway through which individuals attempt to manage psychological distress. Already, the NGS in Ireland has detransitioners who regret their medical treatment. Despite their assiduous checks and safeguards, they were not enough.
Indeed, how could it be? Imagine if national clinics were set up to determine which anorexics would benefit from weight-loss injections and liposuction. They would knock the doors down, desperate to prove they needed these interventions. And the people who would gain access to these interventions would likely be the most extreme – those willing to devote their entire lives to maintaining an identity built on being extremely thin and presenting as extremely well-adjusted in order to convince the doctor that they are a good candidate. The level of commitment required to secure these interventions requires a consuming obsession.
This is what has already happened with medical transition clinics such as the NGS in Ireland and NHS adult gender identity services in Britain. Johns Hopkins reopened its gender service in 2017, nearly four decades after closing it in 1979. What was once a rare and unusual condition has become widespread. We have established this as healthcare without any meaningful evidence base to support it.
For this reason, we need to raise public awareness that if people want to medicalise their identities, this should be understood as a form of extreme body modification. It should not be viewed as healthcare, nor performed in hospitals, but in extreme body modification clinics that make no claim to medical legitimacy. People with diagnosed DSDs should be supported to access whatever healthcare interventions are required to alleviate their condition, but everyone else should be told plainly that they are engaging in a practice that is not healthcare and carries significant and often harmful consequences in the long-term. Facial feminisation can be difficult to live with if it is regretted. Genital surgery can be devastating, to the point that even contemplating regret can lead to suicidality. The stakes are extremely high, and the responsibility on the doctor is immense. Increasingly, that responsibility is being avoided through the turn to informed consent.
A compassionate and reliable healthcare system must not allow the patient to lead the treatment pathway. Doctors must offer their expertise, and patients must be able to trust that their care is grounded in evidence-based knowledge as well as clinical judgement.
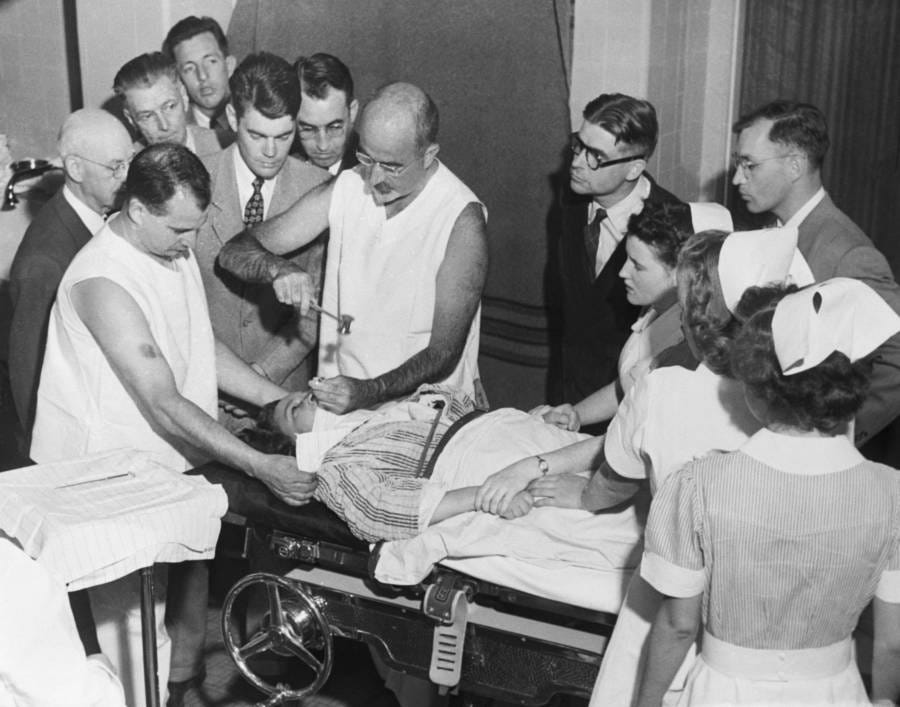
We’ve been here before; medical history is littered with tragedy. The inventor of the lobotomy, Egas Moniz, was awarded the Nobel Prize for his work. Dr Walter Freeman later popularised the transorbital lobotomy, inserting an ice pick through the eye socket to sever the frontal lobes. In his final years, knowing he was dying, he travelled across America seeking reassurance from those who had undergone this procedure. Self-report meant patients and families told him his interventions worked and when he died in 1972, he still believed that lobotomies were the best treatment for mental illness. Yet the long-term outcomes of lobotomy were found to be harmful, and the practice was largely abandoned in the 1970s.
Self-report is not evidence, and belief is not proof. Medicine must be guided by objective outcomes, and in the case of medical transition, the outcomes do not justify the intervention.

